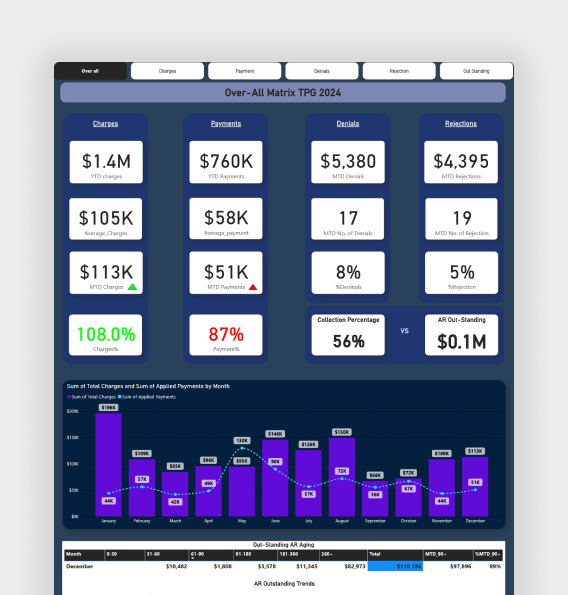
ICS Medical Billing Company provides total visibility into your revenue cycle
Medical Billing Reports & Revenue Cycle Reporting Services
Medical billing reports are essential for healthcare providers to track financial performance, identify revenue gaps, and improve operational efficiency. Without accurate reporting, providers cannot effectively manage their revenue cycle or make informed business decisions.
InfoHub Consultancy Services delivers advanced medical billing reporting and revenue cycle reporting services for healthcare providers across the United States. As an offshore medical billing company in India, we provide real-time reporting insights for hospitals, clinics, physician practices, and healthcare organizations.
Our reporting solutions help providers in California, Texas, Florida, New York, Illinois, and across the USA gain full visibility into their billing performance, collections, denials, and revenue cycle operations.

 Medical Billing
Medical Billing